Mitral Valve Regurgitation Treatment
Treatment for MR aims to limit or stop your valve leakage. It also relieves symptoms and improves the quality and length of your life.
For mild MR, medicine and close follow-up with frequent echocardiograms are often all you need.
But because MR is a mechanical problem with blood flow, valve repair or replacement is often best.
Doctors at the UPMC Center for Heart Valve Disease are experts in minimally invasive and surgical techniques for repairing your mitral valve.
Your doctor will use the approach that best meets your needs.
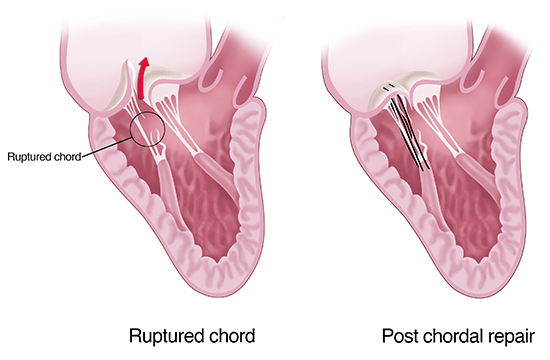
Mitral valve regurgitation occurs when the valve separating the left heart chambers doesn't close properly and allows blood to leak backward through the mitral valve. Treatment involves surgically repairing or replacing the mitral valve.
Valve repair surgery for mitral regurgitation
The first line treatment of MR, especially for mitral valve prolapse, is valve repair surgery.
This involves surgery to restore your mitral valve's normal function by rebuilding your existing flaps. We tailor the technique to your anatomy.
At the UPMC Center for Heart Valve Disease, we do this operation every day with a repair rate of over 90%.
Benefits of minimally invasive mitral valve surgery
Minimally invasive approaches make a small incision on the front of the chest or the right side of the chest.
These smaller cuts to access the heart lead to:
- Less pain and blood loss.
- Reduced risk of infection.
- Faster recovery, allowing you to get back to your life sooner.
After mitral valve repair surgery, most people:
- Get off the breathing machine quickly, sometimes while still in the OR.
- Stay in the hospital for three to five days before going home.
- Can do some activities the first three to four weeks post-op. But avoid heavy lifting and driving. Your doctor will explain what you can and can't do.
After three to four weeks of recovery, you can slowly return to normal healthy activity, including driving.
Minimally invasive robotic-assisted mitral valve surgery
UPMC is a leader in minimally invasive robotic mitral valve repair.
This allows the surgical team to access the mitral valve directly — often through a 2-inch incision — with technical and imaging precision.
It's the preferred treatment for people with isolated MR due to mitral valve prolapse.
Compared to some other types of surgery, robotic mitral valve repair:
- Avoids disturbance to the ribs or chest.
- Causes less pain.
- Allows for a faster recovery and return to your daily routine.
Transcatheter Edge-to-Edge Repair (TEER)
UPMC is one of the few centers in southwestern Pa. to offer transcatheter edge-to-edge repair, a minimally invasive approach to MR valve repair.
Experts at UPMC's Center for Heart Valve Disease perform this procedure through a vein in the leg. The surgeon passes a catheter with the clip into the heart to bring the mitral valve's two flaps together.
UPMC uses two commercially available systems: Abbott's MitraClip System and Edwards' Pascal Precision System. Surgeons often use the TEER technique to treat people who are too high risk for heart valve surgery.
Mitral valve replacement surgery
Mitral repair is always our first approach, especially for those with degenerative or "floppy" valves.
But we may perform a mitral valve replacement for moderate to severe cases of MR.
This occurs if repairing the valve isn't an option because of:
We replace the mitral valve with a valve made of either metal flaps (mechanical) or cow or pig tissue (biologic).
- Metal valves are long-lasting but require you to take a blood thinner, warfarin (Coumadin®), for life.
- Tissue valves don't last as long as metal ones but often don't need lifelong blood thinners. Depending on your age and condition at the time of surgery, tissue valves may eventually need replacement.



















